HHT symptoms
HHT is a hereditary vascular disease caused by a shortage of specific proteins which help stabilize blood vessel walls. That is why HHT causes vascular abnormalities (malformations).
Since all the blood vessels are subject to the same hereditary deficiency, these abnormalities can occur anywhere in the body. However, there are predilection sites, such as the skin on the face and fingers, and the mucous membranes of the nose, mouth and digestive tract.
The organs and tissues most affected bij HHT are:
- Brain
- Skin, mucosa and nails
- Liver
- Lungs
- Stomach and intestines
- Nose
- Eyes
- Spine
Symptoms per organ/tissue
Brain (CAVM)
HHT of the brain may lead to epilepsy, headache and haemorrhage, but not to migraine.
Brain (cerebral) vascular malformations (CAVM) occur more often in HHT-1(10%) than in HHT-2 (approx. 1%), like pulmonary vascular malformations. The precise frequency is not known because large numbers of patients have not been screened and because screening methods are not 100% sensitive. CAVMs may vary from small telangiectases to AVMs (arteriovenous malformations) of several centimetres. They can occur everywhere in the brain and there are multiple CAVMs in about one-third of HHT patients. Usually, they do not cause complaints, but epilepsy, headache and haemorrhage may be present. Migraine is not a symptom of a CAVM, but of a pulmonary AVM. CAVMs are usually detected by routine screening of adults and sometimes of children.

Screening
There is considerable debate about the necessity to screen for CAVMs. In the USA, they tend to screen all HHT patients. In Europe, opinion is more diversified. First of all, the chance of finding a CAVM is much smaller in HHT-2 than in HHT-1. Secondly, the screening methods are not perfect and treatment is not always possible or may be complicated. Thirdly, the risk of haemorrhage seemed to be only 0.5% – 0.7% per year in a French and a Dutch study, but was 1.4% - 2% per year in an English study.
Young patients with HHT-1 should certainly have screening for CAVM, particularly when they have symptoms. An individual approach is required in other groups of patients.
Skin, mucosa and nails
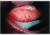
Telangiectases appear as little red dots of several millimetres and disappear when compressed. These lesions particularly appear on the face, finger tips and the mucous membranes of the lips, tongue, mouth and sometimes the eyes. Very small telangiectases are often present in the cuticles. They can be seen under a microscope. They are easily recognized by an expert, but may be missed by inexperienced doctors. It is also possible that an incorrect diagnosis of HHT is made on account of false telangiectases.
The lesions have a thin wall and are located superficially. Therefore they bleed easily. Occasionally there are larger elevated abnormalities. When required (in case of frequent bleeding or severe cosmetic objections) treatment is relatively easy with electro-coagulation or laser treatment.
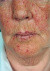
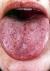
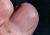

Telangiectasia on the skin, tongue, cuticle and nail bed
Prevalence of teangiectases in skin and mucosa
The typical telangiectases usually start to appear after puberty and increase in number with aging. Virtually all HHT patients have these lesions as adults.
Liver
Vascular abnormalities of the liver due to HHT (HAVM) may vary from small telangiectases to very large AVMs, which may accommodate 50% of the blood that flows through the body (cardiac output).
Symptoms
Small liver AVMs do not cause complaints and are often detected because laboratory analysis has disclosed abnormal liver values. However, large AVMs can cause fatigue from failing liver function or abdominal pain after meals. The latter is caused by the fact that the bowels require more blood to digest the meal, but the amount of blood is limited because so much flows through the liver AVMs.
A delusive complaint is shortness of breath. The heart normally pumps 5 litres per minute through the body. This cardiac output may increase to 10-15 litres in the case of large liver AVMs. The high cardiac output can cause high blood pressure in the pulmonary arteries, cardiac enlargement, and shortness of breath.
Prevalence of HAVMs
The liver is probably affected very often, particularly in women and in patients with HHT-2. A liver biopsy is therefore dangerous and is not advisable for any HHT patient, unless there is a very strong indication. The diagnosis is made by ultrasound (echography), CT scan or angiography. An ERCP – a small catheter is introduced via the stomach into the bile ducts to visualize them – is also dangerous.
Lungs
The vascular abnormalities of the lung can vary from small telangiectases to very large AVMs up to 10 centimetres. These are called pulmonary AVM (PAVM). When left untreated AVMs of the lungs may cause cerebral abscess and infarction.
Usually, multiple PAVMs are present at the base of one or both lungs.
Symptoms
PAVMs lack capillaries just like other AVMs. The capillaries of the lung are important because they ensure the addition of oxygen to the blood and because they filter the venous blood which often contains small clots, debris and clumps of bacteria – even in healthy persons. Normally these cannot pass the lung because of this filter and cannot reach vulnerable organs like the brain. The symptoms of a PAVM are largely the result of these missing capillaries:
Shortage in oxygen
No oxygen is added to the blood at the site of the PAVM, and the lung veins that drain the PAVM will contain too little oxygen, making a so-called shunt. This oxygen-poor blood mixes with the oxygen-rich blood that has passed the pulmonary capillaries. The mixture that the heart pumps to other organs such as the brains, intestines and skin will contain less oxygen. This shortage of oxygen may manifest itself as:
- blue colouring of the skin and lips (cyanosis)
- shortness of breath
- broadening of the finger tips (clubbing)
However, the shortage of oxygen is usually only minor and is experienced as ‘poor physical fitness’ or ‘fatigue’. The patients are used to these symptoms and often do not consider them as abnormal.
'Leakage' of the cappilary filter
Because the capillary filter is absent at the site of the PAVM, blood clots or bacteria can pass through the lung. This material passes to the left side of the heart and is pumped to the brain etc. This can lead to a:
- transient ischemic attack (TIA): a temporary interruption in the blood flow to the brain (symptoms disslove within 24 hours);
- brain infarction: a blockage of a blood vessel in the brain causing a part of the brain tissue to die;
- brain abscess: a collection of infected material in the brain, caused for example by bacteria or fungi;
- migraine with aura: severe headaches accompanied by seeing flashing lights and hearing noises.
Cerebral complications are thought to occur in 40-50% of the patients with an untreated PAVM.
Bleeding (haemorrhages)
The third complication that can occur is a bleeding in the chest cavity or airways due to rupture of the PAVM. This is very dangerous but rare; it occurs in 2 to 3 % of the pregnancies. Most often, blood in saliva is not the result of a ruptured PAVM, but of the aspiration of blood from the nose or the bleeding of small telangiectases in the airways.
Prevalence of PAVMs
PAVM do occur in children, but they are usually found only after puberty. In the Netherlands 29% of HHT patients under the age 18 had a PAVM in 29%. In adults they are found more often in HHT-1 (48%) than in HHT-2 (5%) and more often in women (65%) than in men (35%). They can grow particularly during pregnancy or if a patient also has a specific heart disease. Female hormones may play a role.
PAVMs occur relatively frequently and may be dangerous. However, treatment is usually effective.
Stomach and intestines
Telangiectases and small AVMs
Telangiectases and small AVMs can occur in the entire gastrointestinal tract, but are most commonly located in the stomach and the beginning of the small intestines. There are often many telangiectases.
Symptoms
HHT of the digestive tract does not cause abdominal complaints, nor does it lead to pain, heartburn or constipation. It does often cause anaemia. Chronic mild bleeding is often present in middle-aged patients. Possible symptoms are:
- black stools, because of
- chronic mild bleeding in the digestive tract;
- swallowing of blood coming from the nose or
- taking iron supplements.
- aenemia
- fatique
The suspected diagnosis should be confirmed by endoscopy or video capsule, because HHT patients, just as people without HHT, can also have an ulcer, polyps or cancer.

Prevalence
Telangiectases and sometimes small AVMs are present in the digestive tract in about 25% of HHT patients.
Nose
Telangiectases and sometimes small AVMs are nearly always present in the nose and cause the most common complaint in 95% of HHT patients: spontaneous and sometimes severe nose bleeds. The abnormalities in the nose bleed more easily than those of the skin, because they are more vulnerable. This is due to their position between the soft mucosa and the hard cartilage. The nose bleeds usually start around the age of 10 years and increase with age.
Spontaneous nose bleeds in a child of a parent with HHT should raise suspicion of the presence of HHT, but they are no proof. Children without HHT can also suffer nose bleeds. Examination by an experienced ear, nose and throat (ENT) specialist is necessary. On the other hand, although 20% of HHT-1 and 46% of HHT-2 patients under the age of 21 years do not suffer nose bleeds, the ENT specialist can still detect telangiectases. The absence of nose bleeds does not prove the absence of the disease.
Symptoms
Severe nosebleeds may cause:
- anaemia
- fatigue
Prevalence and severity of nosebleeds
The frequency and severity of the nose bleeds differ from patient to patient. One-third of the Dutch patients have them daily, including at night. So, they interfere with sleep. They last for a short period (1-5 minutes) in 50% of cases, but for more than 15 minutes in 10% of cases.
Luckily the nosebleeds are rarely fatal, but they may be very inconvenient, especially in social situations. A recent questionnaire showed that 22% of the Dutch patients considered their quality of life to be affected by the nose bleeds.
What causes nosebleeds
Nosebleeds are often caused by injury of the vascular abnormality by:
- dry air (air-conditioning, travelling by plane),
- nose picking
- colds
- sneezing (allergy), or
- excessive use of nasal decongestants.
Eyes
About 20% of HHT patients have telangiectases in the mucosa of the eyes, on the inside of the eyelids. These can bleed. The retina has been studied systematically only once. The study showed that 10% of patients had retinal abnormalities, without complaints.
Spine
AVMs of the spinal cord are present in less than 1% of the patients. They usually cause symptoms in childhood. Symptoms include:
- paralysis;
- pain and
- in rare cases transverse lesions.
An MRI should be done if there are any symptoms.
