Examination and treatment
In patients with HHT all the blood vessels are subject to the same hereditary deficiency. Therefore the vascular abnormalities caused by this deficiency can occur anywhere in the body. However, there are predilection sites, such as the skin on the face and fingers, and the mucous membranes of the nose, mouth and digestive tract.
The organs and tissues most affected bij HHT are:
- Brain
- Skin, mucosa and nails
- Liver
- Lungs
- Stomach and intestines
- Nose
- Eyes
- Spine
Click on one of the items below for more information on examination methods to diagnose and treatments to treat vascular abnormalities in that particular organ or tissue.
Examination and treatment per organ/tissue
Brain
Examination
The best screening method is the MRI scan with gadolineum, but small lesions may be missed. Angiography of the cerebral blood vessels is performed to prove their existence and to study the architecture, when an MRI scan gives rise to suspicion of an AVM.
Treatment
The size and architecture of the CAVM determine whether treatment is indicated. The aim of the treatment is to prevent haemorrhage and may consist of radiotherapy, embolisation or operation. The results are usually good.
Skin, mucosa and nails
Examination
Telangiectases in the skin, mucosa and nails. They appear as little red dots of several millimetres and disappear when compressed. They are easily recognized by an expert, but may be missed by inexperienced doctors.
Very small telangiectases are often present in the cuticles. They can be seen under a microscope. This so-called capillaroscopy – visualization of the capillaries – is a painless examination which takes only a few minutes. It may contribute to the diagnosis.
Treatment
When required (in case of frequent bleeding or severe cosmetic objections) treatment is relatively easy with electro-coagulation or laser treatment.
Liver
Examination
The diagnosis of HHT in the liver is made by:
- ultrasound (echography);
- CT scan or
- angiography.
An ERCP – an examination method in which a small catheter is introduced via the stomach into the bile ducts to visualize them – is dangerous for HHT patients.
Treatment
Treatment is only needed in the case of very large liver AVMs.
Embolization is not a good option because fatal complications have been reported. However, good results were published by a German clinic recently. Surgical removal is not possible. Sometimes a liver transplantation is the only possibility in severe cases. These patients should be assessed in a specialised centre.
Bevacizumab (see nose) has been used in a few patients with good results.
Lungs (PAVM)
Examination
PAVMs can be diagnosed by doing:
- a chest X-ray;
- an echo bubble test
- an angiography
- an X-ray of the blood vessels of the lung filled with injected contrast fluid.
The chest X-ray only shows large PAVMs and smaller ones are often missed. The shunt can be demonstrated by measuring air bubbles on an echocardiogram of the heart, the echo bubble test, which are normally caught by the capillaries, but pass though the PAVM. The echo bubble test is the most sensitive and demonstrates even the smallest PAVM’s that cannot be visualised by radiological techniques. Therefore, it often occurs that the echo bubble test shows a shunt in the lungs, whereas the CT-scan shows no PAVM.
The presence of PAVMs is subsequently proven by angiography, an X-ray of the blood vessels of the lung filled with injected contrast fluid.
The size and architecture of the PAVM determine whether treatment is indicated.

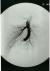
Treatment
Treatment was often a bilateral operation in the past. At present, embolization is the treatment of choice. It is a far less traumatic intervention. In an embolization a catheter is introduced into a vein in the groin and moved through the heart into the feeding pulmonary artery of the PAVM. Small platinum coils or a titanium plug are pushed through and out of the catheter into the feeding artery. The coils or plugs will stay in place, if they have the proper size. A clot will form around this foreign material and the artery is blocked: the PAVM will disappear.


Embolization takes 1 to 3 hours depending on the number of feeding arteries and PAVMs. The patient will need to stay one night in hospital. Sometimes, several embolization procedures are required if there are many PAVMs.
Check-up
A check-up is needed to detect reperfusion or the formation of new PAVMs in time. The first check-up is 6 months after embolization, then, if everything looks good, after 3 or 5 years.
Results
Embolization of the pulmonary arteries is not a common procedure, and therefore requires an experienced interventional radiologist. Results are often good: the PAVM is permanently blocked in 90% of cases, and the oxygen pressure rises.
Reperfusion of the PAVM occurs in 10% of the adult patients and in 30% of the children. It usually requires another embolization.
The procedure is well tolerated, although the patient has to lie for several hours on a hard operating table. Patients may experience some chest pain due to irritation of the lining of the lung (pleurisy).
Prophylactic antibiotics
Every patient with a PAVM, embolized or not, and every patient in whom PAVMs have not been excluded should take prophylactic antibiotics if they need an unsterile intervention, such as dental surgery or incision of abscesses. Such interventions often lead to the presence of bacteria in the blood stream, which may pass through remaining microscopic PAVMs and cause a brain abscess. The instructions for prophylactic antibiotics are given in the chapter about special surgery and anaesthesia.
Stomach and intestines
Examination
In the stomach and intestines the diagnosis is made by endoscopy: the inspection of the mucosa via a tube introduced through the mouth or the anus. Another technique is the photographic video capsule. A small capsule is swallowed and travels through the digestive tract taking flash photographs twice per second. Thousands of photographs are transmitted digitally to a receiver that is attached to the abdomen. Subsequently, the photos are viewed via a computer.
Treatment
Treatment usually consists of supplementing the iron stores of the body by taking iron preparations. Sometimes, blood transfusions are required. In these cases, it is preferred to try to localise and laser the bleeding lesions with endoscopy. However, the results are modest, because there are usually many lesions, of which several may be beyond the reach of the endoscope. The so-called double balloon endoscopy has a larger reach than the ordinary endoscopy. An operation is rarely indicated.
Treatment with female hormones or thalidomide (Softenon) is an entirely different option. They often improve the bleeding, just like the nose bleeds, but may lead to severe side-effects and are not considered lightly.
Nose
Examination
Spontaneous and severe nose bleeds in a child of a parent with HHT should raise suspicion of the presence of HHT, but they are no proof. Children without HHT can also suffer nose bleeds. Examination by an experienced ear, nose and throat (ENT) specialist is necessary. On the other hand, although 20% of HHT-1 and 46% of HHT-2 patients under the age of 21 years do not suffer nose bleeds, the ENT specialist can still detect telangiectases. The absence of nose bleeds does not prove the absence of the disease.
Tips to prevent nosebleeds
Nosebleeds are often caused by injury of the vascular abnormality by dry air (air-conditioning, travelling by plane), nose picking, colds, sneezing (allergy) or excessive use of nasal decongestants. To prevent them the following can help:
- Humidification with saline solutions or humidifying creams such as Sofradex.
- Not picking.
- Careful nose blowing and sometimes anti-allergic drugs may be useful.
- Maintaining a normal blood pressure. A high pressure in the feeding blood vessels of the nose can precipitate bleeding, e.g. high blood pressure, exercise, strain, sex or stress. Maintaining a normal blood pressure is therefore important.
- Foods and drinks: some foods or drinks may aggravate nosebleeds in certain individuals, for example alcohol, spices, foods high in salicylates (including red wine, spices, chocolate, coffee, and certain fruits), natural antiplatelet activity (garlic, ginger, ginseng, ginkgo biloba, and vitamin E15), or omega-3 acids (oily fish, salmon).
- Spongostan, “Heltiq Bloodstop”, “Rapid Rhino”, Merocel tampons, a cut vaginal tampon, ephedrine nose ointment often help to stop the bleeding. But often these are not covered by the insurance.
Drugs that interfere with coagulation, such as aspirin, ascal etc. are contra-indicated, but may be necessary because of thrombosis etc.
More information
A brochure about the treatment at home of the nose bleeds is available (Hart & Vaatgroep; St. Antonius Hospital; see organisation and addresses).
Treatment
The treatment of the nose bleeds is not easy at all and the results are often disappointing because of their recurrence. Treatment always causes injury to the nasal mucosa, which may lead to the formation of new telangiectases. The adage ‘to do as little as possible for as long as possible’ still holds true. The assessment of whether to treat or wait should be made by an experienced ear, nose and throat specialist. Expert treatment should be given only in serious cases, such as persistent anaemia not caused by telangiectasia of the intestines, social isolation, or disability.
The ear, nose and throat specialist has the following options:
- Coagulation, preferably by Argonplasma laser beams because they cause less injury than electrical or chemical cauterisation. General anaesthesia is often necessary.
- Transplantation according to Saunders with Ross modification. This involves replacing the diseased nasal mucosa by normal skin tissue under general anaesthesia.
- Correction of the nasal septum or concha when the air flow seems to injure the mucosa.
There are also non-operative options:
- The contraceptive pill, e.g. Neocon. It is not known exactly why the contraceptive pill works, but it is recognised and experienced by many HHT patients. The long-term use of the contraceptive pill has several drawbacks and balanced consideration and a regular check-up by the general practitioner are required. A history of breast or uteral cancer or thrombosis is a contra-indication. However, the contraceptive pill sometimes proves to be the best solution for women with severe nose bleeds. The contraceptive pill is not an attractive treatment for men because of the side effects.
- Aminocaproic acid, a drug that promotes coagulation of the blood, may help in cases of severe nose bleeds. However, it could also promote thrombosis elsewhere in the body.
- Acetylcystein (Fluimucil ), 3x 600 mg daily. Oxygen radicals are involved in the bleeding in laboratory animals. Acetylcystein inactivates these radicals. A recent Dutch trial shows that the nosebleeds indeed diminish. The product is safe and without side-effects. It is not covered by all insurance companies.
- Embolization under local anaesthesia is another alternative. The feeding blood vessels of the nose are blocked with artificial material by a catheter that is introduced through the groin. It should be considered only when other treatments have failed. Temporary results are good but new blood vessels will eventually appear. It requires an experienced interventional radiologist.
Eyes
Examination
To determine if a patient has telangiectases in the eyes a HHT specialist examines the inner side of the eyelids.
Treatment
About 20% of HHT patients have telangiectases in the mucosa of the eyes, on the inside of the eyelids. These can bleed, but can be effectively treated with coagulation.
Spine
AVMs of the spinal cord are present in less than 1% of the patients. The diagnosis is made with MRI. An MRI should be done if there are any symptoms. Treatment is often possible in specialised centres.
Epidural anaesthesia is given through a needle that stays out of the vertebral canal and complications are not expected.
Intra-dural anaesthesia is given through a needle in the vertebral canal, which can puncture a spinal AVM. However, the chance of an AVM is less than 1%.
Check-ups
Adult patients with only abnormalities of the skin and mucous membranes are advised to have a check-up every five years in order to see whether their internal organs remain unaffected.
Adults with a localisation in the lungs, brains, stomach, intestines or liver, are advised to have a yearly to five-yearly check-up, depending on the types of lesions and type of treatment, as long as their condition is stable.
Children, who do not seem to be affected, should be re-examined around puberty and when they turn 18 years. Children with a vascular abnormalities in the lung should have a check-up more frequently or every five years if there are no lung abnormalities.
